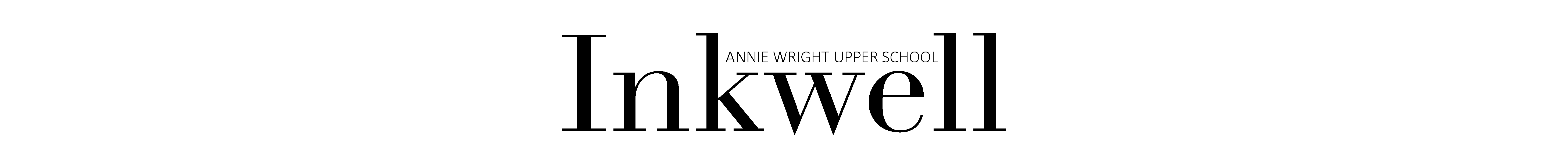A Perspective from the Front Lines of the COVID-19 Pandemic
photo courtesy of Sofia
Medical staff wear scrubs, as well as white coats, to ensure no outside contaminants or pathogens are carried via clothing.
April 24, 2020
As of now, there are over 1,000 confirmed COVID-19 cases in Pierce County, Washington. Medical professionals continue to work on the front lines while risking exposure each day in their endeavors to mitigate this pandemic. Among these front liners is Miles Ching, a nocturnist, or night shift hospitalist, working for Franciscan Health at St. Joseph’s hospital in Tacoma.
On a daily basis, Ching sees around four-seven patients of varying degrees of COVID-19 risk. He described his personal protection equipment protocols based on risk. “When I see a patient who is not suspected of having COVID-19, I will always have a surgical mask, an eye shield, then an N95 underneath my surgical mask, and rubber gloves as well,” Ching said. An N95 mask is a type of respiratory protection equipment that is designed to fit the face of its wearer and acts as an effective filter, blocking 95% of 0.3 micron test particles. It is recommended by the CDC as a sufficient protective measure against COVID-19.
In addition to low-risk cases, Ching also sees patients suspected of having COVID-19 and those who have already tested positive. When he sees these patients, Ching wears a disposable gown and a CAPR. A CAPR is a type of face shield made of plastic that covers the face, creating a seal. It also includes a helmet that creates positive air pressure, pushing air out of the system and preventing particles from entering. “It limits any droplets from coming in contact with my face, and it also limits any droplets from entering in the openings, which significantly reduces any chance of exposure or contracting COVID-19.”
As a nocturnist, Ching’s shift lasts from 8:30 pm to 8:30 pm. “During my shift, I’ll see probably four-five [newly admitted] patients, plus check up on additional one-two already admitted patients, looking at symptoms, like a drop in blood pressure, shortness of breath…Throughout my twelve-hour shift, I will probably spend four or so hours at the bedside with a patient, communicating with the nurse,” Ching reported. During these hours spent in the hospital, Ching and other front liners are at a constant risk of exposure.
In addition to the hours spent in the hospital, Ching also works for eight or so hours in his office. “Actually, most of my time is spent documenting and writing orders for these patients, answering phone calls about the patients, from the office,” he said. However, even while in a large and relatively safer space, Ching must always wear personal protective equipment like a surgical mask and maintain a distance of at least six feet between himself and all other colleagues.
Working as a front liner has resulted in the integration of near-extreme sanitary measures into Ching’s everyday life. “When I arrive at the hospital, there is just one entrance that we use. They will always screen us for temperatures and symptoms, and hand us a mask to use.” Throughout the day, Ching washes his hands frequently and sanitizes the boot and scooter he uses due to a healing foot fracture.
The sanitation process Ching undergoes returning home is even more elaborate. “It’s quite an ordeal, leaving the hospital,” he said. “When I get to the car, I sanitize everything again. When I arrive home, the first thing I do is leave the shoes and the boot I wear in the hospital outside of the house, then I take off all the dirty clothes and throw them in the wash. From there, I shower straight away. I don’t come in contact with my family till after.” These practices have become essential in keeping Ching and his family as safe as possible.
Recently, Ching has been ordered to self-isolate as a result of potential exposure to a confirmed COVID-19 case. Because the patient was not initially suspected of COVID-19, Ching had only the lesser level of personal protective equipment, excluding a gown and CAPR. “The patient came in with an unusual presentation. She didn’t have any cough, no shortness of breath; she just had bleeding. But on review of the history, three weeks prior she was exposed to COVID-19 and did have symptoms at the time.”
There are three levels of exposure that are taken into consideration when someone is advised to self-isolate. The first is low risk, which is usually described as a situation in which only some small protective measures are not taken. Medium risk can be characterized by the lack of a major protective measure, such as an eye shield or mask for a patient or doctor, with an extended exposure time. A high risk exposure occurs when no personal protective measures are taken.
Ching’s exposure is considered low risk. His self-isolation requires that he wear a mask when outdoors and closely monitor for any fevers, coughing, sore throat, or other symptoms for fourteen days following his exposure. “I am still able to work at the office, but must be careful to limit contact with patients.”
Despite the gravity of his situation and role in the pandemic, Ching keeps his morale up by devoting himself to his work. “The good thing about going to work and seeing patients that need your help is knowing that you really do have a purpose,” Ching explained. “It helps for me not to stay home the whole time, to go out and do something about this.”
“It was difficult in the beginning when we still didn’t have the equipment to treat the patients. The only downside there was to helping was when we simply didn’t have enough equipment to help with. But it really has gotten a lot better, and the community is a big help.” Ching expressed gratitude for the community’s action in providing resources for hospitals. As an example, his own daughter helps by hand sewing masks from cotton shirts.
“We do what we can,” Ching stated. “It may be frightening and difficult, but we do what we can.”